Predict heart failure from cardiac CT scans 86% accurately and offer a 5yr risk score for earlier care
Oxford researchers show that AI can predict heart failure from cardiac CT scans by reading subtle signals in fat around the heart. In a 72,000-patient study, the tool flagged risk up to five years early with 86% accuracy, offering doctors a clear score to guide closer monitoring and prevention.
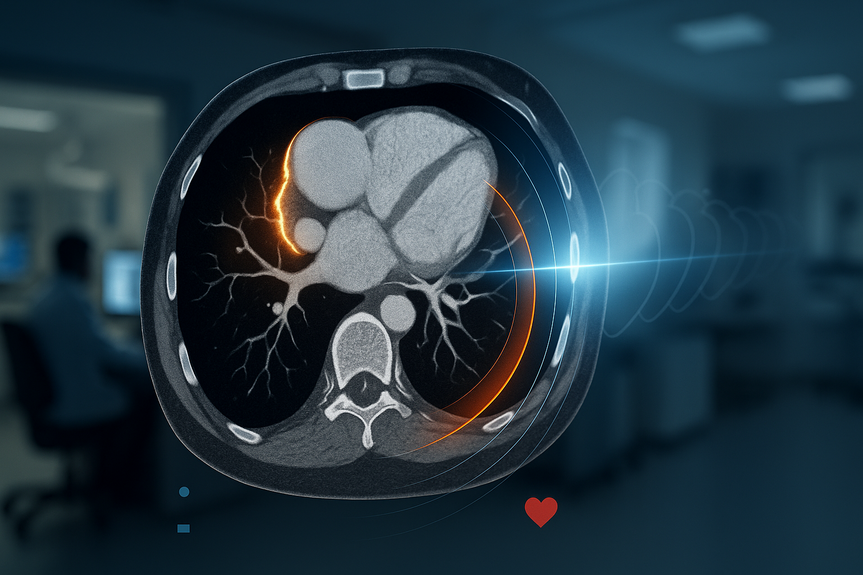
Heart failure affects millions of people and often shows up late. Doctors need a way to see risk earlier and act sooner. A new AI tool from the University of Oxford offers that early warning. It reads regular CT scans, studies fat around the heart, and finds signs of hidden inflammation that humans cannot see. These signals help doctors spot who is at high risk and who needs closer care now.
How AI can predict heart failure from cardiac CT scans
The signal in heart fat
CT scans capture more than arteries. They also capture the fat that wraps the heart. When the heart is under stress or inflamed, the nearby fat changes. The AI measures tiny texture and brightness patterns in this fat to judge if it is healthy or not. These patterns act like a thermometer for the heart.
Training and accuracy
Researchers trained and tested the system on 72,000 patients from nine NHS trusts in England. Each person had a cardiac CT and at least 10 years of follow-up. The AI predicted who would develop heart failure within five years with 86% accuracy. It gave each patient a simple risk score that doctors can use to plan care.
Key findings from the study
People in the highest risk group were 20 times more likely to develop heart failure than those in the lowest group.
About one in four people in the highest group developed heart failure within five years.
The tool worked on routine cardiac CT scans, without extra tests or manual input.
Results were published in the Journal of the American College of Cardiology.
How hospitals could use it
Turning scans into action
A risk score can guide simple but important steps:
Flag high-risk patients for closer follow-up and repeat checks.
Start or adjust medicines earlier, such as for blood pressure or diabetes.
Refer sooner to heart failure clinics for echo scans or specialist care.
Support lifestyle changes with clear, personalized risk communication.
This method helps care teams predict heart failure from cardiac CT scans during routine imaging for chest pain or suspected artery disease. The Oxford group aims to extend the approach to any chest CT, even scans done for other reasons. That could catch risk in more people, including those scanned for lung issues.
What this means for patients
Earlier warning, better choices
If doctors can see risk five years ahead, they can act before the heart weakens. People may avoid emergency hospital visits and severe symptoms. A clear score can also help patients understand why changes matter and stay on track with medication, exercise, and checkups.
Even today, many hospitals can predict heart failure from cardiac CT scans if this tool sits inside standard radiology software. It would run in the background and add a line to the report that says how high the risk is and what steps to consider next.
Limits and next steps
Regulatory approval is pending before wide rollout, including in the NHS.
Sites outside England will need validation to confirm accuracy in other populations.
The tool predicts risk; it does not replace a diagnosis or a doctor’s judgment.
Prospective trials should test whether using the score reduces hospitalizations and deaths.
What you can do today
Build everyday heart strength
Eat more fruits, vegetables, whole grains, and beans.
Move at least 150 minutes a week; add strength work twice weekly.
Keep a healthy weight and waist size.
Quit smoking; avoid secondhand smoke.
Limit alcohol; choose alcohol-free days each week.
Check and control blood pressure, cholesterol, and blood sugar.
Ask your doctor what your CT scan shows and if follow-up is needed.
Know symptoms: breathlessness, leg swelling, fatigue, rapid weight gain, or chest pressure.
Strong prevention still matters. But when routine scans can also act as early alarms, more people can stay ahead of trouble.
In short, this study shows how AI can predict heart failure from cardiac CT scans and give doctors and patients a crucial head start. With careful rollout, clear oversight, and smart use in clinics, it could change how we prevent and manage heart failure.
(predict heart failure from cardiac CT scans)
(Source: https://www.theguardian.com/society/2026/apr/08/oxford-scientists-develop-ai-tool-spot-heart-failure)
For more news: Click Here
FAQ
Q: How does the Oxford AI tool predict heart failure from cardiac CT scans?
A: The tool analyses the fat that wraps the heart on routine cardiac CT scans, measuring tiny texture and brightness patterns that indicate inflammation not visible to the human eye. Using those signals it produces an absolute risk score and can flag people at risk up to five years before heart failure develops.
Q: How accurate is the AI and what study supports its performance?
A: Researchers trained and validated the system on 72,000 patients from nine NHS trusts in England who had at least ten years of follow-up, and it predicted five-year risk with 86% accuracy. The results were published in the Journal of the American College of Cardiology.
Q: What does being in the highest risk group mean for a patient?
A: People in the highest risk group were 20 times more likely to develop heart failure than those in the lowest group, and about one in four in that group developed heart failure within five years. Doctors could use that score to prioritise closer monitoring and earlier interventions for those patients.
Q: Does the tool require extra scans or manual input to work?
A: The study found the method works on routine cardiac CT scans without extra tests or human input, allowing it to run alongside standard radiology analysis and add a risk line to reports. The Oxford team is also working to adapt the approach to any chest CT performed for other reasons to identify more at-risk people.
Q: Can this AI replace a doctor’s judgement or make a diagnosis?
A: No, the tool predicts future risk but does not replace a clinical diagnosis or a doctor’s judgement. It is intended to inform monitoring and care decisions rather than serve as a standalone diagnostic test.
Q: What regulatory or validation steps are needed before the tool is widely used?
A: The team is seeking regulatory approval to roll the tool out in healthcare systems including the NHS, and sites outside England will need validation to confirm accuracy in other populations. Prospective trials are also needed to test whether using the score reduces hospitalisations and deaths.
Q: How might clinicians act on a patient’s risk score in practice?
A: Clinicians could flag high-risk patients for closer follow-up, order echocardiograms or specialist referrals sooner, and start or adjust medicines for blood pressure or diabetes. The score can also support targeted lifestyle advice and clearer conversations with patients about prevention.
Q: What can patients do now to reduce their risk of heart failure?
A: Standard prevention remains important: eat more fruit and vegetables, be physically active, maintain a healthy weight, stop smoking, limit alcohol, and control blood pressure, cholesterol and blood sugar. Patients can also ask their doctor about their CT scan results and seek follow-up if they have symptoms such as breathlessness, leg swelling, fatigue or chest pressure.